GLP-1
XM-S (GLP-1 Pathway)
GLP-1 receptor agonist peptide for metabolic and appetite research.
View product →
GLP-1
XM-T (Dual Pathway)
Dual GIP and GLP-1 receptor agonist for metabolic research applications.
View product →
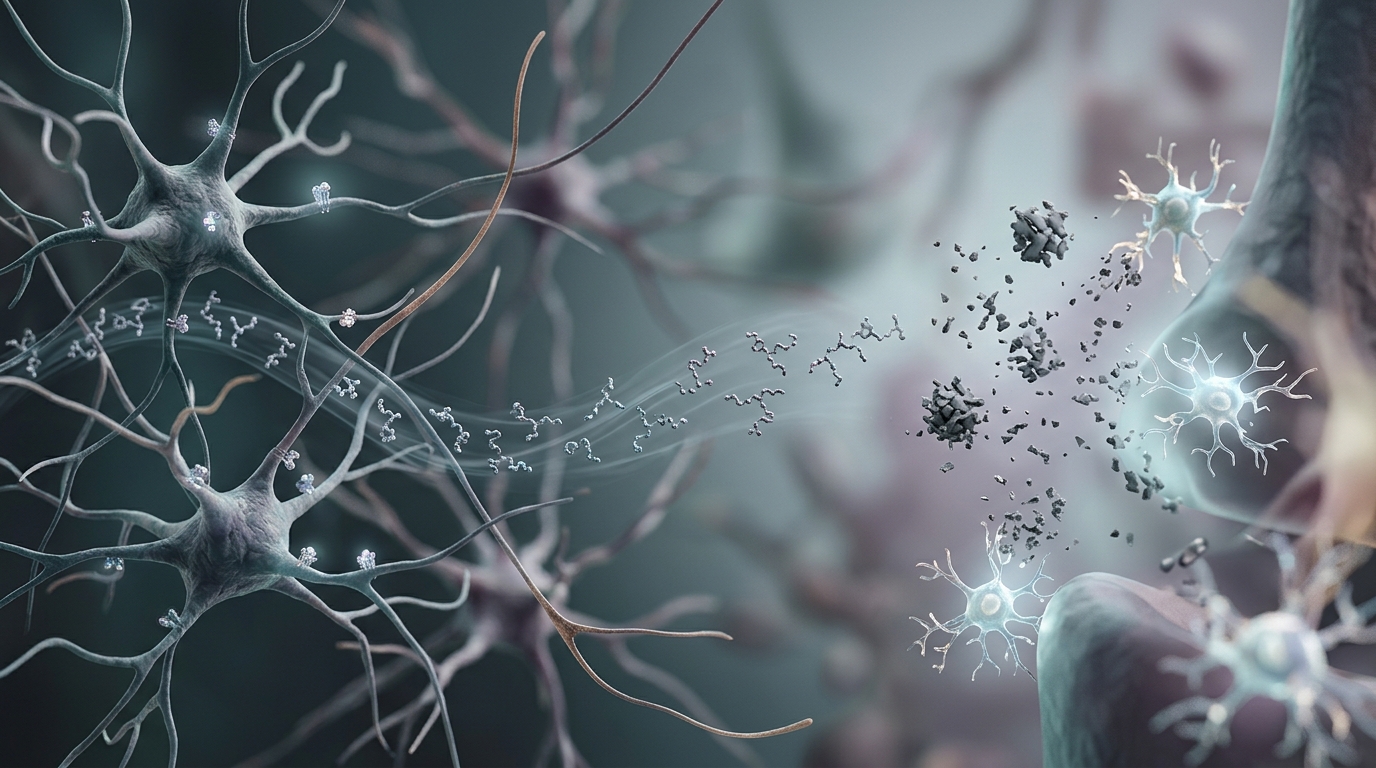
Glucagon-like peptide-1 (GLP-1) receptor agonists and related incretin agents have attracted attention beyond metabolic endpoints because of emerging evidence that they engage central pathways implicated in neurodegeneration. Studies suggest these agents influence amyloid processing, tau phosphorylation, neuroinflammation, mitochondrial function, and synaptic plasticity — mechanisms directly relevant to Alzheimer’s disease pathology and, by extension, Alzheimer’s risk. Pharmacology of GLP-1 agents relevant to the brain GLP-1 receptor (GLP-1R) is a class B GPCR expressed in the periphery and in discrete central nervous system (CNS) populations, including the nucleus tractus solitarius, hypothalamus, hippocampus, and cortex. Agonism of GLP-1R increases intracellular cAMP, activates PKA and PI3K–Akt pathways, and can engage MAPK/ERK signaling; downstream effects include modulation of cellular metabolism, transcriptional programs for survival, and anti-apoptotic signaling. Receptor occupancy and functional potency are typically reported in the low nanomolar range for clinical GLP-1 analogs, but CNS effects depend on pharmacokinetic properties such as half-life, plasma AUC, and blood–brain barrier (BBB) permeability. Large-peptide GLP-1R agonists differ in molecular weight, albumin- or Fc-binding modifications, and enzymatic stability (notably resistance to DPP-4), producing a wide range of systemic half-lives from hours to days. CNS penetration can occur via saturable transport, transcytosis at circumventricular organs, or modulation of vagal afferent signaling rather than direct parenchymal receptor engagement. Thus, central pharmacodynamics may reflect both direct receptor activation in brain tissue and indirect effects mediated by peripheral metabolic changes (insulin, lipids, inflammatory mediators) that secondarily affect the CNS. Mechanistic pathways linking GLP-1R signaling to neuroprotection Multiple mechanistic axes provide a biological plausibility for GLP-1 agonists to influence Alzheimer’s-related processes. Key pathways include: Reduction of neuroinflammation: GLP-1R activation attenuates microglial and astrocytic proinflammatory signaling in rodent models, lowering cytokine production (IL-1β, TNF-α) and shifting microglia towards phenotypes associated with debris clearance rather than chronic activation. Mitochondrial and metabolic stabilization: cAMP/PKA and PI3K–Akt signaling downstream of GLP-1R can stabilize mitochondrial membrane potential, reduce reactive oxygen species production, and enhance mitophagy and bioenergetic reserve in neurons. Amyloid and tau modulation: Preclinical data indicate changes in APP processing enzymes (BACE1), reductions in Aβ oligomer levels, and decreased tau phosphorylation via glycogen synthase kinase-3β (GSK-3β) inhibition pathways. Synaptic function and neurogenesis: GLP-1R signaling promotes long-term potentiation (LTP) and dendritic spine density in hippocampal circuits and enhances markers of adult neurogenesis in dentate gyrus niches. These effects are mechanistically coherent with reduced vulnerability of circuits that undergo early Alzheimer’s-related degeneration, notably the hippocampus and entorhinal cortex, and provide multiple targets for readouts in translational studies. Preclinical evidence in Alzheimer’s disease models Rodent and nonhuman-primate studies have assessed GLP-1R agonists across genetic and toxin-based Alzheimer’s models. Data indicate consistent effects on behavioral endpoints (spatial memory, contextual fear conditioning) and biochemical endpoints (reduced plaque burden, lowered soluble Aβ oligomers, and attenuated tau hyperphosphorylation). Several studies show preserved synaptic markers (synaptophysin, PSD-95) and reduced markers of oxidative stress after chronic GLP-1R agonist exposure. Timing of intervention matters: preventive or early-intervention paradigms produce larger effect sizes than late-stage treatment in most models, suggesting GLP-1–mediated mechanisms are more effective at halting progression or reducing vulnerability than reversing extensive established pathology. Pharmacokinetics and regimen considerations in animal studies Preclinical regimens use a range of administration routes (subcutaneous, intraperitoneal, intracerebroventricular) and formulations with varying systemic half-lives. Reported half-lives span minutes (native GLP-1) to days (acylated or albumin-bound analogs), with corresponding differences in AUC and steady-state exposure. Intracerebroventricular dosing demonstrates that direct central receptor engagement recapitulates many benefits seen with peripheral dosing, supporting a central mechanism component; however, peripheral metabolic changes (improved insulin sensitivity, reduced peripheral inflammation) also account for part of the neuroprotective signal. Careful PK/PD matching and measurement of central exposure (CSF concentrations, brain homogenate levels) are critical for interpreting translational relevance. Clinical and epidemiologic evidence linking GLP-1 agents to Alzheimer’s risk Observational studies have reported associations between use of GLP-1 receptor agonists (and related incretin therapies) and reduced incidence of dementia diagnoses in people with type 2 diabetes, with hazard ratios suggestive of lower Alzheimer’s risk after adjustment for metabolic confounders in some cohorts. Such studies are susceptible to confounding by indication, immortal-time bias, and differing follow-up durations; nonetheless, the directionality across multiple datasets has prompted prospective investigations. Randomized controlled trials (RCTs) evaluating metabolic outcomes have occasionally reported cognitive or neuroimaging secondary endpoints. These data are limited by short durations (typically 6–52 weeks for cognitive measures), underpowered cognitive batteries, and variable baseline cognitive status. A small number of trials deliberately enrolling older adults or individuals with mild cognitive impairment are ongoing or recently completed, with readouts focusing on amyloid/tau PET and CSF biomarkers as well as cognitive composite scores. Preliminary trial reports and pooled secondary analyses indicate modest improvements or attenuated decline on some cognitive measures, but results are heterogeneous and require replication in adequately powered, dementia-specific RCTs. Comparative CNS pharmacology: semaglutide, dual-agonists, and next-generation molecules Not all GLP-1–based agents are pharmacologically equivalent with respect to CNS engagement. Structural differences — acylation site, albumin binding affinity, molecular size, and additional receptor targets (GIPR, glucagon receptor) — influence receptor selectivity, systemic half-life, and potential BBB translocation. For example, small structural modifications can alter GLP-1R affinity in the nanomolar range and change agonist efficacy (full vs partial agonism) and biased signaling tendencies (favoring cAMP vs β-arrestin pathways). Tirzepatide, a dual GIP/GLP-1 receptor agonist, produces distinct metabolic effects compared with selective GLP-1 agonists and could theoretically engage additional CNS pathways through GIPR expressed in brain regions. Comparative preclinical head-to-head studies report differing magnitudes of neuroprotective endpoints across compounds, but direct translation requires matching for central exposure and receptor occupancy. Biomarkers and imaging endpoints suitable for trials targeting Alzheimer’s risk Biomarkers provide mechanistic and proximal endpoints to assess whether GLP-1–based interventions modulate pathways relevant to Alzheimer’s disease. Key measurable endpoints include: CSF biomarkers: Aβ42/Aβ40 ratio, total tau, phosphorylated tau (p-tau181, p-tau217), and neurofilament light chain (NfL) for neuroaxonal injury. Molecular PET: Amyloid PET (e.g., 18F-florbetapir) and tau PET (e.g., 18F-flortaucipir) for in vivo pathology quantification and regional progression tracking. Functional imaging: FDG-PET for metabolic patterns, amyloid-related hypometabolism, and fMRI for connectivity and task-related activation changes, particularly in default-mode and hippocampal networks. Peripheral markers: Plasma p-tau, plasma Aβ species, inflammatory cytokines, and metabolomic signatures that may reflect central processes or downstream peripheral effects. For prevention-oriented trials, sensitive cognitive composites (e.g., Preclinical Alzheimer Cognitive Composite) paired with longitudinal biomarker change (CSF and PET) provide a pragmatic approach to detect early disease modification before overt clinical dementia. Pharmacodynamic readouts (CSF drug concentration, receptor occupancy surrogates) help disentangle central vs peripheral mechanisms. Safety signals, confounders, and translational gaps Safety profiles of GLP-1R agonists are well-characterized in metabolic populations and include gastrointestinal effects, pancreatitis signals (disputed and rare), and potential for gallbladder-related events; CNS-specific adverse events are infrequently reported but deserve close surveillance in older populations. Importantly, peripheral metabolic improvements (weight loss, improved glycaemic control, lipid changes) may themselves reduce Alzheimer’s-related risk, acting as mediators rather than direct central effects. Disentangling mediation from direct neurobiology requires trial designs with target engagement biomarkers and appropriate control arms. Key translational gaps include: Clear measures of central exposure: CSF or brain concentrations are reported in limited datasets; many trials lack PK measures to relate systemic dosing to central receptor occupancy. Heterogeneity of Alzheimer’s pathophysiology: subgroups defined by amyloid status, APOE genotype, metabolic profile, or vascular burden may respond differently. Duration and timing: given the decades-long natural history of Alzheimer’s disease, the optimal window for intervention (midlife metabolic correction vs late-life disease modification) remains to be defined. Research priorities and recommended trial designs To determine whether GLP-1–based therapies modify Alzheimer’s risk, randomized, sufficiently powered trials with disease-specific endpoints are required. Recommended elements for future trials include: Enrollment stratified by baseline amyloid/tau status and APOE genotype to evaluate heterogeneity of treatment effect. Primary endpoints combining sensitive cognitive composites with longitudinal biomarker change (CSF p-tau, amyloid/tau PET) and plasma biomarkers to enable earlier signal detection. Pre-specified mediation analyses to separate peripheral metabolic effects (weight, insulin resistance) from central biomarker changes. PK/PD substudy to quantify CSF exposure, receptor occupancy surrogates, and pharmacodynamic markers in peripheral blood and CSF. Longer follow-up (multi-year) with interim biomarker analyses and adaptive features to enrich responders or extend follow-up in signal-positive subgroups. Combination trials evaluating GLP-1 agonists with agents targeting complementary mechanisms (anti-amyloid immunotherapy, tau-directed agents, anti-inflammatory compounds) could clarify whether GLP-1–mediated changes enhance or synergize with disease-specific interventions. Conclusions Preclinical data and emerging epidemiologic signals provide a biologically plausible rationale that GLP-1 receptor agonists and related incretin agents may reduce Alzheimer’s risk via multiple central mechanisms — anti-inflammatory, metabolic, anti-amyloid/tau-modulating, and synaptic-supportive pathways. Current clinical evidence is suggestive but not definitive: observational studies indicate lower dementia incidence among treated patients, and early clinical trials report mixed biomarker and cognitive readouts. Definitive answers require randomized, biomarker-rich trials with careful PK/PD measurement, stratification by Alzheimer’s-relevant risk factors, and sufficiently long follow-up to capture disease-modifying effects. All discussion here is intended for preclinical and translational research contexts; these data do not constitute clinical recommendations or endorsement of self-administration.