Peptides That Accelerate Bone Repair: Preclinical Evidence and Protocol Guidance
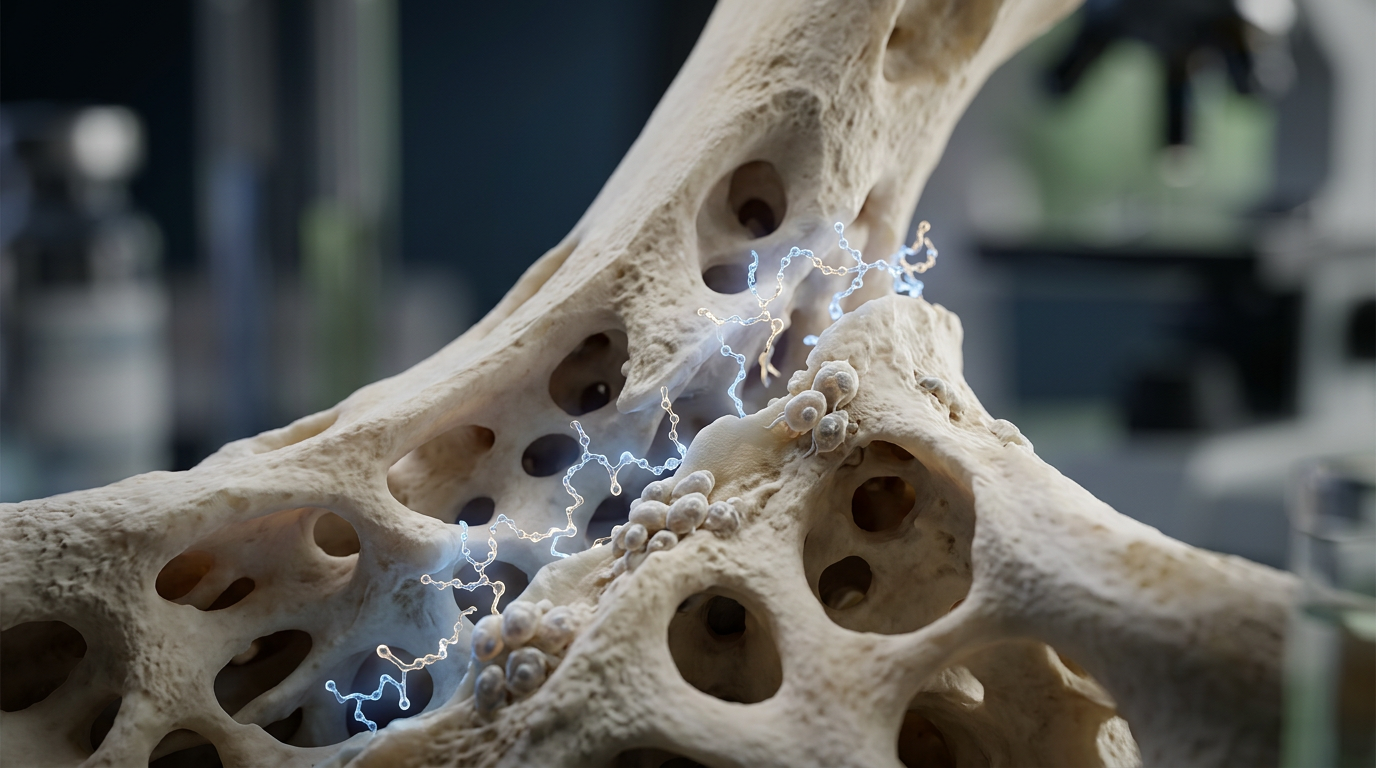
When a postdoc in a university orthopedics lab swapped a saline control for BPC-157 in a femoral defect model, the first histology slide told a quick story: thicker callus, more osteoid, earlier bridging. The lab didn't stop there. They layered angiogenesis markers and micro-CT timepoints to build a reproducible protocol. That bench-side narrative—the small change that sharpened an endpoint—is the practical thread of this article.
Why consider peptides for bone repair? Bone healing is a cell- and signal-driven process. Inflammatory signals recruit cells. Vascular sprouts deliver oxygen and minerals. Osteoprogenitors lay down matrix, then mineralize. Peptides are attractive in preclinical models because many act directly on one or more of these steps: chemotaxis, angiogenesis, osteoblast proliferation, or matrix modulation. They are small, synthetically accessible, and, in many cases, stable enough for repeated dosing in rodents. For labs focused on mechanism or improving time-to-union in animal models, peptides provide a modulatable toolkit that sits between growth factors (large, complex proteins) and small molecules.
Core biological mechanisms targeted by recovery peptides Understanding mechanism narrows experimental design. Peptides relevant to bone repair typically influence one or more of these processes:
Angiogenesis — new vessel formation to support callus remodeling. Cell migration/chemotaxis — recruiting mesenchymal stem cells (MSCs) and osteoprogenitors to the injury site. Osteoblast proliferation and differentiation — increasing matrix deposition and mineralization. Inflammation modulation — shortening the catabolic early phase without blocking necessary signaling.
Choose peptides that match the mechanism you want to probe. If your endpoint is early vascular invasion, prioritize angiogenic peptides; if you care about mineral density at 8 weeks, prioritize osteoanabolic signals.
Peptides with notable preclinical data for bone or soft-tissue repair Below are peptides commonly used in rodent and rabbit fracture models. This is not exhaustive; rather, it highlights candidates with multiple independent preclinical reports.
BPC-157 — small, gastric-derived pentadecapeptide reported across multiple rodent studies to enhance tendon and bone healing, often with faster callus formation and improved biomechanical strength in defect models. Thymosin beta-4 (TB-500) — promotes cell migration and angiogenesis; used in muscle, tendon, and some bone models to enhance vascularization and reduce fibrosis. IGF-1 LR3 — long-acting IGF-1 analogue that stimulates osteoblast proliferation and matrix production in vitro and in vivo models. MOTS-c and mitochondrial peptides — emerging data suggest roles in cellular energetics that can affect repair, but bone-specific evidence is still sparse. Myostatin inhibitors / GDF-8 antagonists — while primarily studied for muscle growth, reducing myostatin signaling can indirectly affect bone through increased mechanical loading and paracrine interactions.
Two peptides that appear frequently in practical fracture studies are detailed in the next sections.
BPC-157: preclinical profile and experimental uses BPC-157 (Body Protection Compound-157) is perhaps the most-cited peptide for soft-tissue and bone repair in small-animal work. Multiple groups report faster healing in tendon and bone defect models, with histologic evidence of earlier collagen organization and radiographic signs of bridging at earlier timepoints than controls. Mechanistically, BPC-157 is associated with enhanced angiogenesis, modulation of local inflammatory profiles, and improved fibroblast/osteoblast activity in injured tissue.
Practical notes from published protocols and lab practice:
Route: most rodent work uses intraperitoneal or local peri-lesional administration; intravenous use is less common due to short peptide half-life in small animals. Timing: repeated dosing in the first 1–2 weeks post-injury is common, reflecting the peptide's influence on early inflammatory and angiogenic phases. Endpoints: micro-CT bone volume, biomechanical three-point bending, and histomorphometry are standard to capture structural and functional improvement.
Thymosin beta-4 (TB-500): angiogenesis and migration in repair models Thymosin beta-4 is a 43-amino-acid peptide that promotes cell motility and blood vessel formation. In musculoskeletal studies it tends to improve neovascularization and reduce scarring; those effects can accelerate the provisional matrix organization that precedes bone deposition. TB-500 is often paired with scaffolds or local delivery in bone defect models to maximize local concentration and angiogenic drive.
Design considerations when using TB-500:
Delivery method matters: controlled-release from a scaffold can sustain pro-angiogenic activity during the first 2–3 weeks. Combine with osteoinductive cues when the goal is mineralization; TB-500 alone may not increase osteoblast-specific differentiation enough to change late mineral metrics. Measure vascular endpoints — CD31 staining, perfusion imaging, or vessel counts — alongside bone metrics to demonstrate the putative mechanism.
Designing rodent fracture protocols: timing, dosing windows, and endpoints Peptides typically act most strongly during the early to mid stages of repair: inflammation, soft callus formation, and vascular invasion. Match your dosing window to that biology. For example, a 0–14 day dosing window targets cell recruitment and angiogenesis; a 14–28 day window targets matrix maturation and mineralization. Many labs split regimens across those windows to capture both effects.
Study endpoints and timeline (example) Below is a commonly used timeline for a mid-diaphyseal femoral defect in rats. Adjust days and imaging schedule for species and defect size.
Day 0 — Create defect and apply scaffold or local peptide, when used. Days 1–14 — Active dosing phase for peptides that modulate inflammation or angiogenesis; plan serial assessments for early biomarkers. Week 2 — Micro-CT baseline for early callus volume; histology on a subset (if terminal) for cellular infiltration and vessel counts. Weeks 4–8 — Structural endpoints: micro-CT bone volume/BS/TV, mineral density, and mechanical testing (e.g., three-point bending). Week 8+ — Remodeling phase assessments, long-term biomechanical strength, and revascularization completeness where relevant.
Endpoints to include in most protocols:
Micro-CT quantitative metrics (BV/TV, Tb.Th, trabecular number if applicable). Histomorphometry (osteoid area, osteoblast/osteoclast counts, vessel density by CD31 or vWF). Biomechanical testing (max load, stiffness) for functional readout. Serum biomarkers as adjuncts: osteocalcin, ALP, CTX for turnover trends.
Formulation, stability, and handling — practical lab rules Peptides vary in solubility and shelf stability. Lyophilized peptides from a reputable supplier should include a certificate of analysis and a storage recommendation (typically -20°C or -80°C for long term). Reconstitute using sterile bacteriostatic saline or water according to the peptide's solubility profile. Minimize freeze-thaw cycles; aliquot when feasible. When preparing dosing solutions for in vivo work, create single-use aliquots for the dosing period (e.g., 1–2 weeks) and store at 4°C if stability data allow. Protect light-sensitive peptides from exposure. Maintain sterility: use aseptic technique, sterile vials, and syringes; document batch records.
Assays and imaging to demonstrate mechanism Pair functional outcomes with mechanistic assays. If a peptide is hypothesized to act via angiogenesis, don't rely solely on micro-CT. Add perfusion imaging, vessel counts, or endothelial cell markers. If osteogenesis is the mechanism, include markers of osteoblast differentiation (RUNX2, osterix) in histology or qPCR panels.
Micro-CT: high-resolution scans (voxel size ≤ 10–20 µm for small rodents) provide reliable morphometric data. Histology: Goldner’s trichrome, Safranin-O for cartilage-to-bone transition, and immunostaining for CD31 and osteocalcin. Biomechanics: align testing to defect geometry; three-point bending or torsional testing are common for long-bone models.
Safety, confounders, and reproducibility Peptides can introduce confounders if not controlled. Systemic effects (e.g., altered activity or appetite) change mechanical loading and therefore bone healing. Record animal weight, ambulatory behavior, and food intake. Use blinded outcome assessment to reduce bias; predefine primary endpoints and statistical analysis plans. Batch-to-batch variability and peptide impurities are common issues. Always obtain and archive the peptide lot's certificate of analysis, and where possible run a small stability pilot (n=3–5 animals or in vitro assays) when switching lots. Report sequence, purity, supplier, storage, and reconstitution details transparently when publishing.
Translational caveats and open questions Most data for these peptides come from rodent or rabbit models. Scaling to larger animals introduces different biomechanical forces, immune responses, and pharmacokinetics. A peptide that shortens time-to-union in rats may have limited effect in a load-bearing large-animal defect without a delivery system that sustains local concentrations. Gaps in the literature include long-term remodeling outcomes, dose–response curves in larger species, and interaction effects with bone graft materials or systemic factors (age, diabetes, smoking models). Mechanistic clarity also varies: some papers show strong phenotypes but provide only correlative molecular data. Robust translational work will pair functional outcomes with lineage tracing, single-cell profiling, or targeted blockade experiments where feasible.
Practical lab checklist before you start Use the checklist below to reduce avoidable variation. Tick the boxes before you order animals or begin surgeries.
Define primary endpoint (micro-CT BV/TV at week X, biomechanical failure load at week Y). Choose route and dosing window tied to mechanism (local scaffold vs. systemic dosing). Confirm peptide identity, purity, storage, and reconstitution plan with supplier documentation. Plan blinding and randomization, and pre-specify statistical tests and sample size calculation. Include negative and positive controls where possible (vehicle control, scaffold-only, or known osteoinductive agent). Prepare SOPs for sample collection, imaging parameters, and histology sectioning to ensure consistency.
Closing scene Back in that lab, the postdoc standardized the peri-lesional BPC-157 injections, switched to a consistent micro-CT schedule, and added CD31 counts at two weeks. The next manuscript draft showed clearer mechanistic links and a reproducible effect size. The experiment didn't claim clinical benefit. It did what good preclinical work should: paired clear endpoints with plausible mechanism, documented methods, and left the translational questions open for the next study.
All content is intended for research use only. Not for human use or clinical application.